Magnetic resonance angiography (MRA) and computed tomographic angiography (CTA) can also provide an accurate anatomic assessment of lower extremity arterial disease without some of the risks associated with catheter arteriography. In addition, catheter contrast arteriography provides anatomic rather than physiologic information and may be subject to variability at the time of interpretation. Catheter contrast arteriography has historically been the definitive examination for lower extremity arterial disease, but this approach is invasive, expensive, and poorly suited for screening or long-term follow-up testing. One of the most critical decisions relates to whether a patient requires therapeutic intervention and should undergo additional imaging studies. 
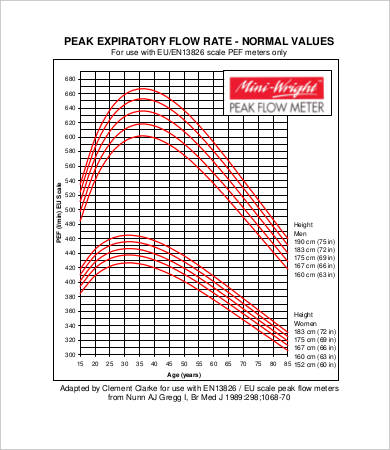
It is therefore necessary when using the above equation for paediatric predicted peak flow, that the value obtained should be converted to the EU scale.Noninvasive testing for lower extremity arterial disease provides objective information that can be combined with the clinical history and physical examination to serve as the basis for decisions regarding further evaluation and treatment. NB: in 2004 the Department of Health initiated a change to PEF meters to align to those that met a new EC standard.The new scale resulted in a conversion being required for PEF recorded using the conventional Wright McKerrow scale to the new European standard.Ī conversion equation was developed by Clement Clarke® that allows conversions of readings from the Wright McKerrow scale to the EN 13826 scale. This applies for ages 15-85 years.Ī paediatric calculation for ages below 15 years is taken from Lung Function by J E Coates (Fourth Edition) and is PEF = 455 x (height/100) - 332. This predicted peak flow calculation is based on the revised Nunn and Gregg equation. However, one study suggested it could be used to rule out severe to very severe COPD, which may be useful if access to spirometry is limited. Peak expiratory flow (PEF) measurement cannot usually be reliably used as the only diagnostic test for chronic obstructive pulmonary disease (COPD) because of its weak specificity. Educating the patient in recognition of symptoms which indicate deterioration is nearly as effective. For patients with stable asthma whose symptoms correlate well with peak flow, a peak flow monitor is adequate. Home monitors which provide FEV1 readings are available and give a more accurate assessment of lung function. There is only low-to-moderate evidence that peak flow readings are related to symptoms. There has been much debate in recent years as to whether routine self-monitoring of peak flow for patients with asthma improves management. However, it still has a part to play if diagnostic uncertainty remains after these tests have been completed. It is less used these days for the initial diagnosis of asthma, clinicians being encouraged to use more accurate measurements of lung function such as spirometry and the fractional exhaled nitrous oxide (FeNO) test. 
Peak flow monitoring is recommended for the ongoing management of asthma and during exacerbations. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
